
Antibacterial sutures stitch the gaps in surgical site infection care
‘Plus’ sutures are reducing the risk of surgical site infections by 28%.
Given that the Asia Pacific region comprises a diverse range of countries with varying climates, cultural, religious, demographic, and healthcare funding landscapes, the distribution of microbial pathogens responsible for surgical site infections (SSI), its prevention, and control within in-patient and post-discharge environments also vary. As such, Johnson & Johnson (J&J) gathered an expert panel of ten stakeholders from the various medical fields across the region and North America for the standardisation of evidence-based practices to improve the surgical outcomes of patients in the Asia Pacific.
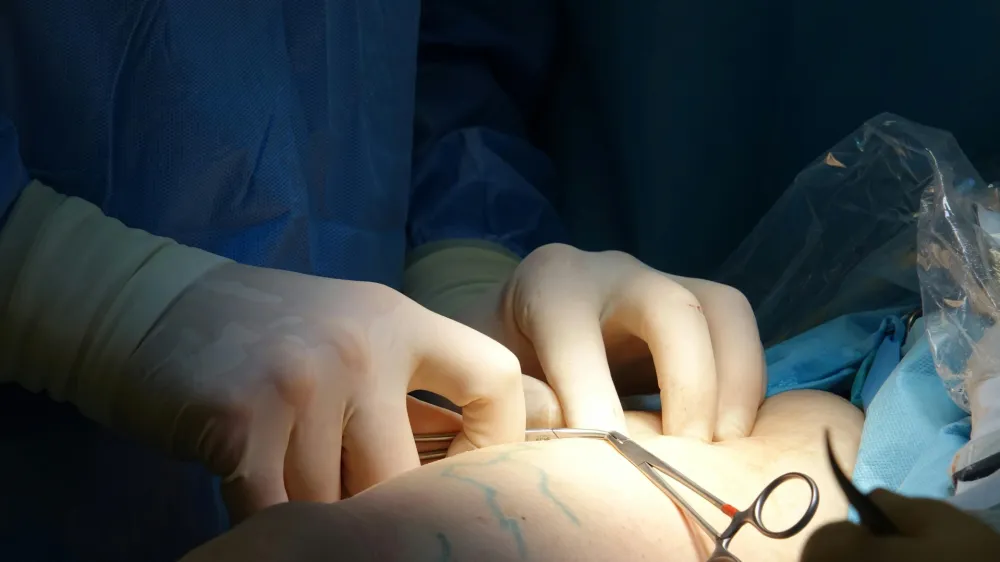
J&J’s solution to reduce SSI is its range of Plus sutures by Ethicon, which contain triclosan, an antibacterial agent which prevents the formation of a biofilm, a known risk factor for SSI. Plus sutures inhibit the bacterial colonisation of the suture for seven days or more against the most common organisms associated with SSI and reduce the risk by 28%.
Healthcare Asia had a conversation with Johnson & Johnson Singapore and Southeast Asia Medical Devices Portfolio Lead Guillermo Frydman on the prevalence of SSIs in the region, and what Plus sutures can do in order to improve outcomes for surgical patients.
Based on your case studies and consumer feedback, how much has SSI affected (a) patient outcomes, (b) economic burden (cost for both patient and hospitals), and healthcare processes (hospital care and home care)?
We found that SSI is the most common postoperative complication through the session conducted with the Antimicrobial Resistance & Infection Control expert commentary. This means that infections at or near the surgical incision are prevalent following an operation, impacting a patient's ability to recover completely and improve their quality of life.
Additional costs are also incurred for both patients and hospitals to treat the infections, putting a strain on healthcare resources to look after patients with SSIs. Research we supported found that for hospitals in Asia, additional costs incurred due to SSI can vary anywhere between US$396 to US$5237 per patient due to prolonged hospital stays, and increased morbidity and mortality following surgery or operation. However, we noted that half of all SSIs could be prevented by implementing standardised SSI prevention guidelines. This will help reduce the risk of infection for patients, length of stay in the hospital, and additional costs incurred due to hospital readmission.
Have standards for SSIs changed during the pandemic, and how?
The pandemic has accelerated the adoption of stricter measures to prevent SSI throughout healthcare systems. Established international guidelines (WHO, US-CDC, the American College of Surgery) have focused on the implementation of continued surgical services and the prevention of SSI in the current climate. These measures are also concurrently implemented with training to differentiate between SSI and COVID-19 infection.
In line with our commitment to support HCPs in the world, we focus on innovative tools such as sutures to help surgeons and patients prevent SSI. Plus Sutures play a vital role in hospital infection prevention measures and help to free up hospital beds with lower readmissions and length of stay.
What difference do Asian SSI patients have with their global counterparts that affect their wound-healing processes?
Asia's reported incidence of SSI varies widely within the region due to the diverse nature of its countries and their healthcare ecosystems – anywhere from 2% to 9.7%. This is significantly higher than in the US, where the incidence rate is just 0.9%.
The challenge in Asia is due to the lack of consistent guidelines for SSI prevention across the region. Some common barriers to adoption include manpower constraints that leave little or no time for training and protocol modifications, limited funding that results in inadequate support for implementing new guidelines, and poor patient awareness and responsibility, leading to increased risk of SSI post-operation.
These are just some challenges that surfaced from the discussion with the expert panel that also recommended that hospitals work actively towards implementing guidelines that apply to them by embedding the relevant SSI prevention programs within their work processes.
What factors and statistical data led you to your innovation of Plus sutures?
At Johnson & Johnson, we understand the ongoing challenges healthcare professionals face and are committed to improving patient outcomes whilst reducing the strain on healthcare systems.
Patients with SSI are twice as likely to spend time in an intensive care unit and five times more likely to be readmitted after discharge. This is a significant strain on both patients and hospitals.
SSIs arise when bacteria colonise the suture material, creating a biofilm as it passes through the skin. This biofilm establishes immunity from both antimicrobial treatment and the host immune system. Once this biofilm develops, there is an increased chance of SSI developing. Research so far has shown that bacteria can colonise monofilament and braided sutures. However, sutures with triclosan can help prevent bacteria colonisation, infections and wound healing disorders.
So far, what results, or outcomes have come from the utilisation of Plus sutures?
Plus Sutures are recommended by several evidence-based organisations, including the World Health Organization, Centers for Disease Control and Prevention, and the Surgical Infection Society due to their triclosan coat.
The National Institute for Health and Care Excellence in the UK has also issued guidance that recommends the adoption of Plus Sutures due to their ability to prevent infections whilst saving costs for patients. In addition, the use of Plus Sutures provides potential environmental benefits to the NHS as a reduced rate of SSIs, in turn, reduces greenhouse gas emissions, freshwater use, and waste generation.
In Singapore, evidence and medical analyses show that Plus Sutures reduce SSI risk by 28% and provide cost savings of $258 per patient compared with using standard non-Plus Sutures. This translates to lower hospital admissions for SSIs following a procedure and more efficient use of hospital resources that can be prioritised for other medical surgeries.
What upcoming plans or projects can you share at this point? What can consumers, patients, and healthcare partners expect from J&J in Asia soon?
Specific to the conversation around surgical site infections, we have recently published two papers developed by a multidisciplinary team of key opinion leaders across the Asia Pacific including surgeons, infection preventionists and C-suite executives. Both publications show a regional consensus on approaching SSI prevention and look at surveillance programs as well as evidence-based guidelines. We hope to reduce surgical site infections in Singapore and the region, to improve patient outcomes while reducing strain on healthcare systems.















 Advertise
Advertise






