Taking a tech advantage on fragility fracture care
The number of hospitals operating on hip fracture that have access to a fracture liaison service has been steadily rising from 2013 to 2020.
In the absence of artificial intelligence (AI) detecting tools, up to 70% of compression fractures can go unnoticed. This calls for an opportunity to use other technology to detect underlying osteoporosis and for earlier intervention, Taipei Medical University’s Department of Radiology chief Wing Chan said in an interview with the Asia Pacific Fragility Fracture Alliance (APFFA) earlier this year..
In Taiwan, Chan has spearheaded the building of a comprehensive fragility fracture care programme at Wan Fang Hospital within the Taipei Medical University. This is comprised of 33 technologists that he has trained personally, APFFA noted in a blog post. Together, their mission has been to standardise and provide quality assurance in osteoporosis care.
In particular, Chan has implemented technology to make it possible to automate the reporting of dual-energy X-ray absorptiometry, which scans bone density to evaluate a person’s risk of breaking their bones. He has also worked hand-in-hand with an IT company to establish AI software that captures compression fractures on CT scans for opportunistic compression fracture analysis.
“There are so many missed cases and signs that we should interpret as osteoporotic, like an empty box appearance, the deformity of the vertebrae, and also some thinning or erosion of the end plate,” Chan said.
In countries such as Taiwan, patients need to pay for their own treatments, unless they have a -2.5 T-score, plus one or more compression fractures. This often means patients go without preventative medication, due to the significant costs they would incur.
“Most of the patients don’t take preventative medication, despite the doctors’ recommendations. In Taiwan, patients are responsible for paying for their own treatment, in the majority of cases, when a compression fracture is not identified,” Chan said.
Such programmes are also in development in Australia. The profile of secondary fracture prevention has been rising in the country, said Jacqui Close, member of the APFFA Joint Steering Committee and co-chair of APFFA’s Hip Fracture Registry Working Group. A report from the Australia and New Zealand Hip Fracture Registry found a steady increase in availability of fracture liaison services over time. The percentage of hospitals operating on hip fracture patients that have access to a fracture liaison service rose to 41% in 2020, compared to just 15% in 2013.
“The roll out of these services varies across Australia's states and territories, with New South Wales having the greatest number of such services,” Close said. “This is a reflection of state policies that have mandated that all health districts in New South Wales have to have a fracture liaison service,” Close said.
Lacking widespread knowledge
However, the country is facing certain challenges in rolling out fracture liaison services across the country. Close noted that the country is still at a stage of having to remind the public and the health system that osteoporosis is a chronic disease that is associated with significant morbidity and mortality, and that it needs to be managed and resourced in the same way as other chronic diseases, such as heart failure and chronic obstructive pulmonary disease.
She also found that the funding arrangements for health in Australia created a challenge particular to the country, with general practice and primary care funded by the Commonwealth government, whilst hospitals are funded by state governments.
“It is the states that bear the brunt of the impact of osteoporosis in terms of managing fractures, yet the responsibility for treating osteoporosis largely sits with the Commonwealth government,” Close said.
APFFA also emphasised the need for better registry data to highlight the challenge the sector faces and the progress it has made over time. The Hip Fracture Registry data revealed that only 37% of hip fracture patients are on treatment for osteoporosis 120 days after their hip fracture, despite medications being widely available through the Australian Pharmaceutical Benefits Scheme.
In Taiwan, the resources available in local hospitals are often limited, making it difficult for clinicians to promote optimal osteoporosis care in local clinics. In the absence of X-ray machines in local hospitals, patients are often referred to larger regional hospitals, and subsequently, can become easily “lost” in the system.
To address the barriers associated with the establishment of a comprehensive fracture care programme, Chan advised for hospitals to adhere to international dual-energy X-ray absorptiometry (DEXA) scanning standards, utilise databases to reach 30% of post-menopausal women who are at risk of osteoporosis, and keep a record of positioning and beta analysis performed by technologists.
He also emphasized the need to invest in an innovation culture and train for an opportunistic ‘capture the fracture’ concept, train colleagues to optimally detect compression fractures, and offer support, passion and consistency.
Wan Fang Hospital granted Chan permission to establish a multidisciplinary clinic in 2019, staffed by physicians across a broad range of specialities, including an endocrinologist, neurosurgeon, orthopaedic surgeon, radiologist, nutritionist, and a clinical nurse who coordinates all patient care.
Across the six clinics, there are currently 700 cases of hip fracture. To date, data has been collected from more than 50,000 cases of quality DEXA reports. Data on body composition, including measurement of the gait, hand grip, and also the nutrition status, is gathered and registered with the hospital’s Osteoporosis and Sarcopenia Care Center.
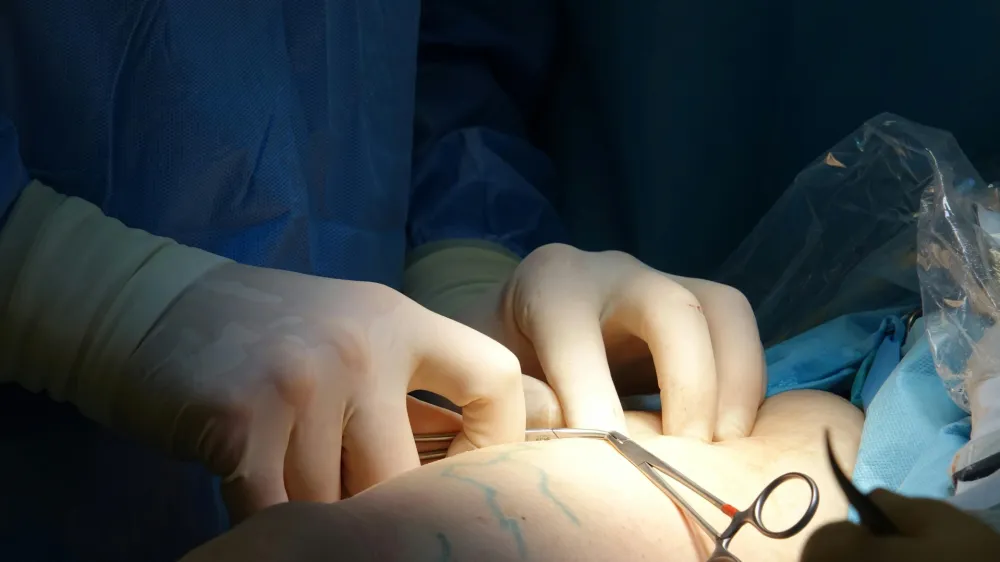
Comeback for orthopedic procedures
The number of orthopedic procedures performed in Australia was estimated to decline in 2020 compared to 2019 due to the pandemic.
A report by GlobalData found that the total number of orthopedic procedures performed in Australia was about 11 million in 2019. About 55% of the orthopedic procedures performed in the country, which include arthroscopy, synovectomy, osteotomy, ostectomy, biopsy, fasciotomy and sequestrectomy, were elective.
“The impact of the Covid-19 pandemic will have many unintended and long term consequences including our ability to provide surgical interventions which significantly enhance the quality of a person’s life and enables them to function and live independently. Arthroplasty is just one example where in Australia we saw a significant reduction in elective procedures during the early phases of lock down,” Close commented.
However, the outlook for 2021 is comparably more promising and optimistic as the number of COVID-19 cases are declining, which will result in a rise in the number of orthopedic procedures performed, especially for elective procedures.
GlobalData’s medical devices analyst Anusha Kaushik noted that a decline in COVID-19 cases is expected to free up beds and reduce the pressure on the country’s healthcare system. This will mean that elective procedures that were delayed or canceled are expected to resume although slowly in the coming quarters.
Close also commented that additional government funds have been made available in Australia to ramp up surgical capacity to address long waiting lists. “This includes incentives for private hospitals to work with the public health system to undertake waitlist reduction programs,” Close added.
Kaushik emphasized that urgent elective procedures are expected to resume first. “This is ultimately expected to lead to a rebound in the number of elective procedures performed,” Kaushik added.
The length of stay at hospitals can be reduced and telemedicine can be used for postoperative visits by the discharged patients. A growing use of new sensor-based wearable technologies will also help in monitoring and managing the patients. “The use of technology is expected to result in more elective procedures being performed as doctors get to spend less time on patient consultations,” Kaushik said.
Across Asia Pacific, the booming medical tourism industry is expected to drive the regional orthopedic devices market, according to a report from ResearchAndMarkets. The higher affordability of orthopedic surgeries in an emerging economy such as India is expected to lure in foreign patients: the country offers healthcare services at a 20% lesser cost than the US, whilst Thailand is 30% lower.
“Such a cost difference is expected to bring a huge clientele to these countries in Asia Pacific, boosting its orthopedic devices market,” the report stated.
Globally, the market for orthopedic devices is expected to reach $59.69b by 2025 from $44.03b in 2020, surging at a compound annual growth rate of 6.3% between the two periods, the report noted. This was attributed to a rise of musculoskeletal injuries with growing participation in sports and an expanding pool of geriatrics, which have become primary undercurrents for the high demand for orthopedic devices.
As the global healthcare system recovers from the pressure of COVID-19, it has been able to increasingly give more attention to elective surgeries. The market also stands to benefit from improving diagnostics that help in identifying osteoporosis fractures and musculoskeletal injuries, the report added.
According to the World Health Organization, about 20-33% of people around the world suffer from musculoskeletal conditions. “This staggering number is an indication that demand for orthopedic devices required for treating hip, vertebral, and forearm fractures will remain high between 2020 and 2025,” ResearchAndMarkets said.
The growing number of sports injuries are also expected to boost the global orthopedic devices market. “Remarkable number of women taking part in sporting activities, upcoming sporting events such as Olympics 2021, and an active lifestyle are expected to result in injuries that will demand orthopedic devices for restoration joints,” the report added.















 Advertise
Advertise






