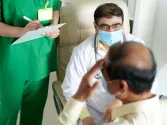
7 ways to boost Indonesia’s healthcare supply chain
The country’s healthcare system suffered from information gaps and a lack of transparency.
The problems in Indonesia’s healthcare system with a fragmented supply chain, information gaps, and lack of transparency have become more obvious as facilities struggled to obtain the supplies required amidst the surging pandemic. Thus, the Australia-Indonesia Centre (AIC) has highlighted seven ways for the country to build a ‘smart’ healthcare supply chain.
The first is to develop an end-to-end digital platform that provides a central view from supply to procurement. AIC’s report noted that digital supply chains are currently fragmented, with different departments in the same hospitals often using different systems. Further, the applications in use appear to be rudimentary and tend not to be integrated.
“Better end-to-end integration of digital supply chains that connect suppliers and upstream processes to a well-integrated internal hospital process is needed. All supply chain processes should be handled through this single platform,” the report stated.
Further, all stakeholders are urged to integrate through a single platform that enables transparent operations and centralised or joint procurement, with all hospitals able to view it in real-time for planning and demand management.
The second way is to have centralised logistics for all government hospitals. AIC found that hospitals in the country currently conduct their own procurement and manage logistics, noting that this is not the most efficient alternative.
“If hospitals under the Ministry of Health can cluster together to manage functions through a centralised digital solution, this would be much more efficient. The shared e-catalogue platform facilitates collective bargaining, but a more holistic logistics solution may improve efficiency, reduce costs, and improve the flexibility of the entire hospital network,” the report added.
Third: ramp up the flexibility of the e-catalogue. AIC said that the inflexibility of government procedures and bureaucratic processes has been hampering the effectiveness of hospitals’ supply chains.
“Whilst the e-catalogue significantly reduces costs for hospitals, the lack of supplier choice can result in long lead-times. It can mean supply is not always available in regional areas. The system should present more than a single supplier and provide flexibility for hospitals to procure from nearby suppliers,” the report added.
Fourth is to make sure there are effective quality and safety monitoring functions. Centrally managed standards are advised to continue being implemented, even when greater flexibility and autonomy for procurement is facilitated in urgent cases.
“Whilst greater flexibility of the Ministry of Health procurement platform will help hospitals obtain supplies efficiently, this needs to be balanced with the quality and safety of any resources,” the report stated.
Fifth, the system must encourage standardisation and interoperability. “Standardisation of supply chain practices and interoperability of digital technologies across the healthcare sector would facilitate better integration and learning, with hospitals better able to share knowledge. This could also facilitate resource-sharing across hospitals,” AIC said.
Sixth, hospitals must ensure transparency and traceability is built into all-digital supply chain solutions, in order to reduce fraud and ensure accountability. “Electronic tagging, robust supplier registration processes and better traceability of the upstream supply chain via systems integration can eradicate counterfeit medication,” the report stated.
Lastly is to develop data analytics capability, which is critical for effective supply chain management.
“Whilst ‘big data analytics’ can significantly affect healthcare supply chains, current analytics seem to be limited to forecasting at best. Real-time solutions, such as real-time streaming analytics, need to be incorporated as part of the future digital solution,” AIC said.
















 Advertise
Advertise