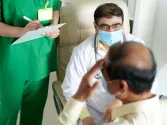
HealthierSG lightens overwhelmed hospitals’ load and reduces healthcare spending
Healthcare reform in Singapore fields general practitioners (GPs) and family doctors to implement preventive care in communities.
With the establishment of ambulatory care centres, some of Singapore’s big hospitals resolved their overwhelmed capacity. This same strategy is applied with HealthierSG, which seeks to place higher focus on preventive care with an ecosystem-based approach that engaged general practitioners and community care centres, offloading the burden from tertiary care hospitals.
“The main idea behind HealthierSG is to shift the emphasis of the health care system from treatment to prevention. In the long run, this will produce better health outcomes for the population at a lower cost. For this to happen, the locus of activity needs to shift from hospitals to community care providers, particularly GPs,” Dr. Alan Ong, principal at Boston Consulting Group (BCG), told Healthcare Asia.
Under the health reform, there are four goals: i) deploying family doctors for preventive care, developing health plans for lifestyle adjustments; ii) regular health screening and vaccinations, activating community partners to lead healthier lifestyles; iii) launching national enrolment exercise for residents to commit to seeing one family doctor and a health plan; and iv) setting up IT and manpower plans as well as financing measures to operate HealthierSG.
Naithy Cyriac, a Partner at YCP Solidiance, said the health reform also helps create a more seamless patient journey. For example, patients will first go to family doctors for preliminary health assessment; and for further consultation, they may be transfered to other tertiary hospitals.
She noted that since some community care centres might not have the most sophisticated medical equipment, a bigger hospital will act on the treatment that will need advanced technology.
“Instead of patients directly going to bigger hospitals, they can go to a family doctor, first, and build that relationship and trust with them,” said Cyriac, in an interview with Healthcare Asia.
Another way that health reform can help big hospitals is to promote the role of primary care through smaller clinics that large private hospital networks have now been focusing on. Cyriac cited Raffles Medical Group, IHH Healthcare, and Fullerton Health as some of the well-known healthcare groups investing in primary care facilities.
“The large private hospital groups are actively engaging their customer base by sharing insights on their website and allowing residents to register interest/ enrol for the HealthierSG initiative easily,” said Cyriac.
The implementation of HealthierSG relies on the national enrolment programme, which will be in phases starting in the second half of 2023. The Ministry of Health (MOH) will encourage residents aged 60 years and above to enroll with a family doctor in mid-2023, followed by those in the 40-59 age group in the next two years.
Lower healthcare spending
A major goal of HealthierSG is to reduce long-term growth in healthcare expenditures. Preventive care is often substantially cheaper than treatment, while also resulting in better health outcomes for the population. Evidence for this comes from systems such as Kaiser Permanente which have a strong emphasis on prevention woven throughout all aspects of their interactions with patients, said Ong from BCG.
However, it is also important to recognise that cost savings will take time to materialise.
Ong said the initial phases of Healthier SG will boost recommended health screening and to increase uptake of regular follow-up and management of chronic diseases.
“This will have a short-term impact of increasing strain on the health care system as more people are found with medical conditions, and more people come forward for the management of their chronic conditions,” Ong said.
“However, in the long run, earlier detection and intervention will result in a lower burden of disease. It is therefore important to plan with an understanding that HealthierSG will take time to show the desired outcomes of lower cost and better quality of life,” Ong explained.
YCP Solidiance’s Cyriac said HealthierSG’s goal of lowering cost is a long-term effect, given the reform’s phased approach.
The idea is that the reform seeks to address vulnerability to chronic disease by enabling patients to have regular annual consultations with their family doctor for early diagnosis and treatment of potential symptoms linked to chronic diseases, Cyriac said.
Doing this would reduce the number of patients diagnosed with chronic illnesses in the long run, resulting in fewer patients in need of long-term care on a five- to ten-year timeline, she said.
One way of lowering the cost of healthcare under HealthierSG is also implementing more affordable drugs. This is where the pharmacist’s cooperation with GPs and family doctors will come in.
“Since more people register with GPs, it will be easier to deliver the screening in a community base. For example, through local clinics, people can receive recommended diabetes screenings to identify patients' health conditions. With the increased screening coverage, patients could be identified at an early stage,” Chia Hsuan Lin, an analyst at GlobalData, told Healthcare Asia.
“It will be essential for GPs and pharmacies to provide medical consultations and personal advice,” added Lin.
Spending on early-stage treatments or moderate to severe treatments is seen to increase and the government’s goal is to control the overall spending, making it more affordable, said Lin. Lowering healthcare expenses will especially help the elderly, who face severe financial burdens since they are the most vulnerable to illnesses.
Amongst the factors that prompted the new health reform is the growing geriatric population in Singapore. One in four residents is expected to reach 65 years old and above by 2023.
Singapore also saw the prevalence of chronic diseases that include hypertension and hyperlipidaemia, which went up to worryingly high levels, at 32% and 37%, respectively.
Notable subsidies, according to Cyriac, include access to fully subsidised recommended screenings (type 2 diabetes, hypertension, breast/cervical/colorectal cancer etc.) and vaccinations (influenza and pneumococcal vaccinations for 65+ years old etc.).
“The first onboarding consultation with the family doctor will be free for residents. Additionally, residents will no longer need to co-pay part of their bills (usually 15%) when opting for MediSave for chronic care management,” she said.
Expenses for yearly check-ins for family doctors will also be subsidised by the government and family doctors will receive an annual service fee, tiered based on health risk profile, scope of needed care, and progress made in preventive care or chronic disease management for the enrolled residents.
“Additionally, to ensure consolidation and sharing of patient health metrics, a one-off grant will also be offered to the primary clinics to encourage digitalisation,” said Cyriac.
GPs that are part of the primary care network (PCN) will also get funding and administrative support from the Ministry of Health (MOH).
“This initiative further incentivises family doctors to join the PCN. In 2018, 340 clinics were part of the PCN and have grown to 670 clinics today compared to about 1,800 clinics in total in Singapore,” said Cyriac.
Digital challenge
HealthierSG’s IT segment will also upgrade digital health apps and wearables to decrease manual tasks and improve health diagnosis. An example of these health apps and wearables is the Healthy365 (H365) app, which has been used by 700,000 residents in the population for the National Steps Challenge and the Eat Drink Shop Healthy Challenge.
Under HealthierSG, H365 will monitor other aspects of healthy living with a diet logging tool that tracks daily caloric intake and provides personalised feedback based on dietary patterns.
But implementing advanced tech may face cybersecurity issues. A 2022 study from Philips Singapore showed that only 23% of Singaporeans are sharing their health data regularly with their doctors or healthcare providers. Amongst their top concerns are data privacy (35%) and a lack of know-how on sharing health data (20%).
HealthierSG can address this challenge first, by giving patients the choice of what data may be shared, said Cyriac. “The data access is fully controlled by the patient, so they can choose what can be shared,” said Cyriac.
Second is, providing a one-time grant or subsidy to help family doctors receive the upgrade and implement the digitalisation processes needed to address privacy concerns.
The MOH is pushing for a framework for the secure collection of health data throughout Singapore’s healthcare ecosystem as embodied in the Health Information Bill still pending approval in the Parliament.
“The bill will mandate licensed healthcare providers to contribute patients’ summarised medical records into the National Electronic Health Record, so as to enable access to patients’ health data by their care teams across different settings. It will also mandate data governance, IT, and cybersecurity capabilities by healthcare providers and data intermediaries,” as mentioned in the whitepaper.
The MOH is also studying provisions in the bill as it will also implement clear and stringent safeguards to ensure proper handling of health information.
Another obstacle to digital apps is encouraging the elderly population to use them. The expansion of eldercare centres (ECs) may help and HealthierSG is seeking to grow the ECs from 119 currently to 220 by 2025.
“ECs provide activities and services for the elderly and the initiative seeks to expand services to include a) community-based monitoring of selected vital signs, b) community connector – to help elderly citizens to sign up for relevant programmes, and c) facilitate uptake of health initiatives such as community health events, basic health screening (dementia, etc.) or end-of-life planning,” said Cyriac.
With the help of the Agency for Integrated Care (AIC), staff at ECs will be trained to improve their capabilities to help in guiding the elderly with digital concerns. The Silver Generation Office (SGO) which already conducts preventive health visits, will also discuss Healthier SG initiatives during these visits to raise awareness. There will also be an improved public infrastructure such as park connectors and sports facilities underway to promote an active lifestyle.
Healthcare staff shortage and training
Implementing healthcare reforms will require more manpower, which is one of the key challenges, said Cyriac. According to the HealthierSG whitepaper, the number of doctors in Singapore grew 50% from 10,200 in 2012 to 15,000 in 2022. For nurses, the number went up by 25% from around 34,500 in 2012 to about 43,000 in 2022.
At present, over 2,600 doctors providing primary care are registered with the College of Family Physicians Singapore (CFPS), of which 1,600 hold a graduate diploma for family medicine at the end of the financial year 2021.
“The Healthier SG initiative recognises the need to increase the number of doctors and nurses in primary and community care from the current one-fifth to at least a quarter by 2030. This is very ambitious and MOH estimates that 3,500 family physicians will be needed by 2030 to facilitate implementation,” said Cyriac.
She also said there is declining interest to pursue family physicians as a career option over specialties.
One way of addressing this is MOH’s plan to collaborate with the CFPS and the relevant Family Medicine training committees, to ensure that all family doctors participating in HealthierSG are accredited as family physicians.
Aside from filling in the shortage, the healthcare reform also seeks to improve interdisciplinary training for nurses and other healthcare professionals to lead community care initiatives.
But Cyriac said that it will be important to identify approaches to expand the number of professionals first before expanding the scope of services for healthcare professionals, who are already strained coming off the COVID-19 pandemic.
Amongst the expansion of healthcare-related education and training opportunities are expansion of the nursing and allied health intakes at the Institute of Technical Education, Nanyang Polytechnic, Ngee Ann Polytechnic, Singapore Institute of Technology, and the National University of Singapore.
The Singapore Institute of Technology also began its nursing degree top-up programme, whilst the Nanyang Technological University opened Singapore’s third medical school.
HealthierSG also wants to increase the number of other healthcare workers such as pharmacists. Since pharmacists will be coordinating with the GPs and family doctors, GlobalData’s Lin said there is still no specific training for pharmacists yet but she said pharmacists’ cooperation with healthcare workers will grow.
“There will be cross-department cooperation to make the whole local-level staff work together. For example, how can local staff trace patients’ health conditions, especially in the situation that people living in the elderly care facilities may not have the time to visit local clinics,” said Lin.
Putting the emphasis on preventive care, HealthierSG will allow pharmacists to lead community care initiatives, take on greater responsibilities and practise at the top of their licenses.
HealthierSG will train more “lay extenders,” which are non-medical personnel who can undertake basic tasks such as arranging the initial health screening, and coordinating referrals to community programmes.
Transformational healthcare
Learning from the COVID-19 pandemic, Ong it is important to ensure that care processes and policies are designed around what works best for patients. This includes thinking through the operational issues that may impact patient experience, such as wait times, the digital interface that patients will have, and the financing gradient from a patient perspective.
For the pharmaceutical market, there will be subsidies and discounts for chronic disease treatments. Lin said the public awareness of chronic disease will increase as patients can receive regular diagnoses to understand their health condition.
“GPS and pharmacists can also provide some medical advice to them. The usage of lifestyle products may increase in a short term due to the increasing accessibility of primary care,” she said.
With the overhaul of the current healthcare system, which focuses on preventive care, Cyriac said it will boost health and quality of life for all Singaporeans in the long term.
“The initiative is a significant step in the right direction and encourages greater collaboration between the healthcare ecosystem to achieve the ambitious KPIs identified such as GP enrolment in the short term, level of physical activity in the medium term, and prevalence of chronic diseases in the long term,” she said.
















 Advertise
Advertise